-
Nieuws Feed
- ECOSYSTEM
- EXPLORE
-
Pagina
-
Groepen
-
Events
-
Blogs
Mild vs Severe Cervical Dystonia Symptoms Comparison: Impact on Daily Life
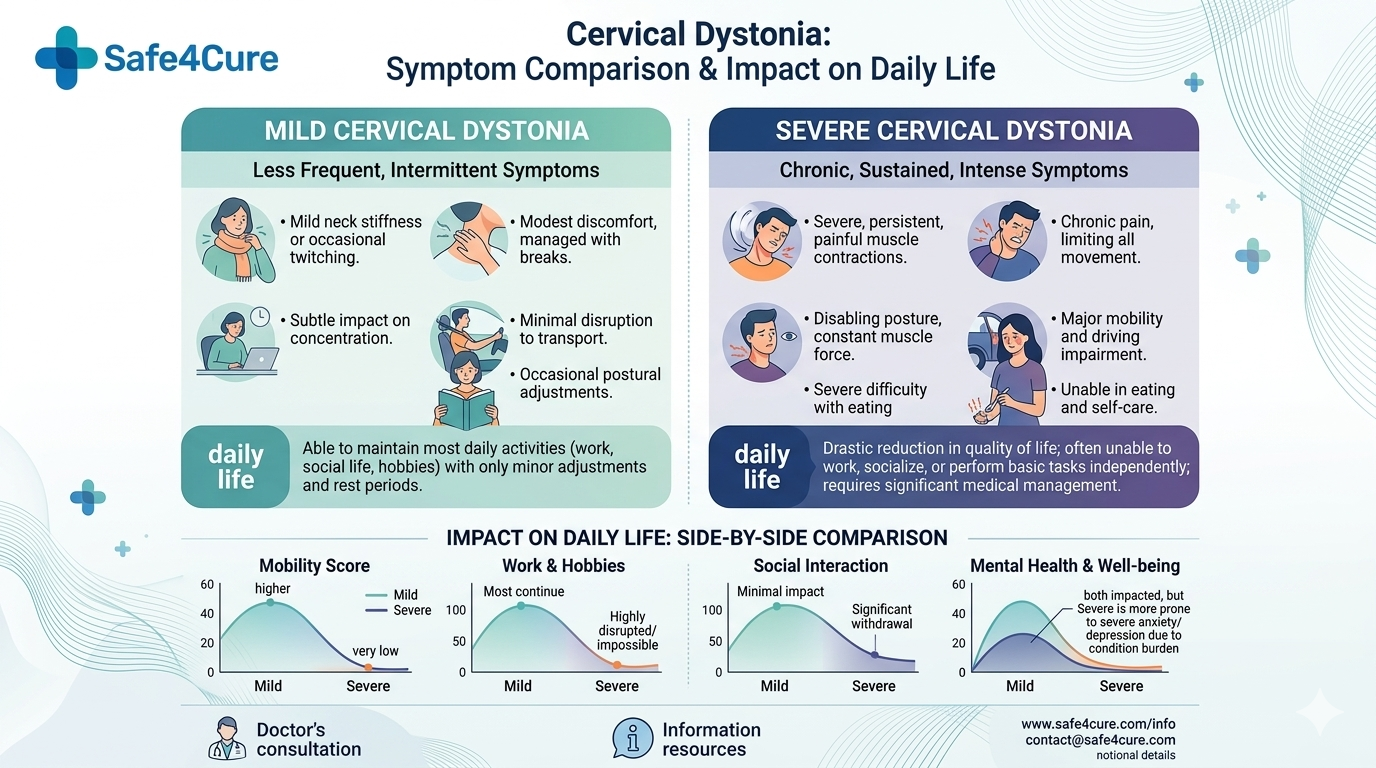
Cervical dystonia, also known as spasmodic torticollis or dystonia of the neck, is a neurological disorder that affects thousands of people each year. It causes involuntary muscle contractions that lead to abnormal head movements and postures. Treatments like Botox Allergan 50 unit treat chin dimpling, cervical dystonia, bunny lips are often used in clinical practice to manage muscle overactivity and improve symptoms. If you have been diagnosed or suspect early signs, understanding the condition is essential for timely management.
The progression of cervical dystonia can vary widely between individuals. In the early stages, symptoms may include mild neck stiffness, occasional muscle spasms, or slight discomfort. However, as the condition advances, these symptoms can become more persistent and noticeable, leading to involuntary twisting, pulling sensations, and abnormal head positioning. This gradual change can make everyday activities more difficult over time.
This guide explains the key differences between mild and severe cervical dystonia symptoms, outlines its meaning and causes, and reviews available treatment options. It also covers important aspects such as Botox duration, therapeutic approaches, and lifestyle adjustments to help improve quality of life and support long-term condition management.
What is Cervical Dystonia? Understanding the Basics
Cervical Dystonia Meaning and Definition
Cervical dystonia is a neuromuscular disorder characterised by involuntary muscle contractions in the neck and shoulder region. The cervical dystonia meaning extends beyond simple muscle tension—it's a complex neurological condition affecting the brain's ability to regulate muscle control.
What is cervical dystonia at the neurological level? The disorder involves dysfunction in the basal ganglia, a region of the brain responsible for coordinating smooth, voluntary movements. When this system malfunctions, the muscles in your neck receive incorrect signals, causing them to contract involuntarily and unpredictably.
Understanding Cervical Dystonia Etiology
The cervical dystonia etiology—the underlying causes and development mechanisms—remains partially mysterious to medical science. However, researchers have identified several important factors:
- Genetic predisposition: Some cases run in families, suggesting a hereditary component
- Neurochemical imbalances: Dysregulation of dopamine, serotonin, and GABA in the brain
- Brain circuitry dysfunction: Abnormalities in the connections between the basal ganglia and motor cortex
- Environmental triggers: Certain traumatic events or repetitive neck strain may activate latent dystonia
- Age of onset: While dystonia of the neck can occur at any age, adult-onset cervical dystonia typically appears between ages 30-60
Cervical Dystonia Causes: What Triggers This Condition?
While no single cause explains all cases, multiple factors contribute to cervical dystonia:
Primary dystonia (idiopathic) develops without an identifiable underlying disease and accounts for the majority of cervical dystonia cases in the United States. Researchers believe this involves genetic mutations affecting neurotransmitter function.
Secondary dystonia can result from:
- Traumatic brain injury or neck trauma
- Stroke or other neurological events
- Medications like antipsychotics (tardive dystonia)
- Parkinson's disease or other neurodegenerative conditions
- Infections affecting the basal ganglia
- Heavy metal poisoning
The exact mechanism of how these factors trigger cervical dystonia remains an active area of neuroscience research.
Early vs Advanced Cervical Dystonia Symptoms: A Detailed Comparison
Mild Cervical Dystonia Symptoms: The Early Stage
Early warning signs before severe cervical dystonia develops are often subtle and easily dismissed as stress or poor posture. Understanding these early indicators can help you seek treatment promptly.
Common Early Presentation:
Mild neck stiffness and postural differences might include:
- Occasional involuntary head turning to one side (torticollis)
- Neck muscles that feel tight or fatigued at the end of the day
- A tendency to favour one side when turning your head
- Mild discomfort that doesn't significantly limit activities
- Symptoms that worsen with stress or fatigue
- Intermittent muscle tremors in the neck region
Early warning signs before severe cervical dystonia develops often appear gradually:
- You notice your head drifting slightly to one side
- Neck tension increases after work or prolonged computer use
- Colleagues or friends comment on your posture
- Pain is minimal, usually ranking 2-3 on a 10-point scale
- Symptoms may be present for weeks or months before diagnosis
Key characteristic of mild cervical dystonia: Many patients report they can perform "sensory tricks" (like touching their face, chin, or head) that temporarily relieve symptoms. This is a hallmark of dystonia and provides immediate, temporary relief during early stages.
Severe Cervical Dystonia Symptoms: Advanced Stage
As cervical dystonia progresses, the distinction becomes clear and increasingly impactful on daily functioning.
Characteristics of Advanced Presentation:
Early vs advanced cervical dystonia symptoms comparison reveals significant changes:
| Aspect | Mild Stage | Severe Stage |
|---|---|---|
| Head Position | Occasional deviation, usually correctable | Constant deviation, fixed or severe |
| Pain Level | Minimal to mild (2-3/10) | Moderate to severe (7-10/10) |
| Sensory Tricks | Highly effective and reliable | Minimal or no effectiveness |
| Tremor | Mild, intermittent | Pronounced, continuous |
| Muscle Tension | Localised to the neck area | Radiates to the shoulders, back, and jaw |
| Functional Impact | Minimal restrictions | Significant daily life disruption |
| Sleep Disturbance | Occasional | Frequent or chronic |
| Work Impact | Manageable | May require work modifications or leave |
Advanced cervical dystonia characteristics:
- Severe, involuntary head turning or tilting that's difficult or impossible to control
- Intense muscle pain and stiffness that persists throughout the day
- Progressive development of secondary complications like headaches, shoulder pain, and arm numbness
- Visible disfigurement or unusual head posture that affects self-image
- Significant functional impairment affecting eating, speaking, or basic hygiene
- Sleep disruption due to pain and involuntary movements
- Psychological impact, including depression and social anxiety
When Mild Cervical Dystonia Requires Medical Treatment
Many people wonder: "Should I seek treatment for mild symptoms?" The answer isn't always straightforward, but certain indicators suggest when mild cervical dystonia requires medical treatment.
Reasons to Pursue Treatment Early
- Progressive nature: Even mild symptoms may worsen over time, making early intervention protective
- Quality of life: Symptoms affecting your comfort or confidence warrant treatment
- Pain and functional limitations: If mild symptoms are causing pain or limiting activities, treatment can improve your situation
- Psychological impact: Social anxiety or self-consciousness about symptoms affects mental health
- Preventative benefit: Early treatment may help prevent progression to more severe stages
When Observation is Appropriate
- Truly asymptomatic or minimally bothersome symptoms
- Normal functional abilities and work performance
- No pain or minimal discomfort
- No psychological distress
Cervical Dystonia Symptoms: Complete Symptom Overview
Motor Symptoms
Involuntary movements and postures:
- Torticollis: Turning of the head to one side (most common presentation)
- Anterocollis: Forward flexion of the head
- Retrocollis: Backward extension of the head
- Laterocollis: Tilting of the head toward one shoulder
- Combinations: Many patients experience multiple movement patterns
Muscle tension and dystonic tremor:
- Course or fine tremor that worsens during directed movements
- Muscle rigidity distinct from Parkinsonian rigidity
- Task-specific dystonia (symptoms worse during specific activities like writing or speaking)
Sensory and Associated Symptoms
- Neck pain: Often the most bothersome symptom, ranging from mild to severe
- Shoulder and back pain: Secondary to abnormal posturing
- Headaches: Particularly at the base of the skull
- Jaw and face pain: From compensatory muscle tension
- Numbness or tingling: In arms or hands from muscle compression
Non-Motor Symptoms
- Fatigue from constant muscle tension
- Sleep disruption
- Difficulty concentrating
- Anxiety and depression (common psychological responses)
- Social withdrawal due to embarrassment about appearance
Cervical Dystonia Treatment: Your Complete Options
Non-Pharmacological Treatments
Cervical Dystonia Exercises
Physical therapy and targeted exercises play a crucial role in cervical dystonia management, though the approach differs from typical neck strain therapy.
Effective cervical dystonia exercises include:
-
Gentle Stretching Regimen
- Slow, sustained neck stretches in all directions
- Shoulder rolls and scapular stabilisation exercises
- Holds are maintained for 30-60 seconds without forcing
-
Proprioceptive Training
- Exercises that enhance body awareness
- Mirror feedback exercises to identify dystonic patterns
- Postural awareness training
-
Relaxation Techniques
- Progressive muscle relaxation
- Breathing exercises (diaphragmatic breathing)
- Yoga and Pilates adapted for dystonia
-
Sensory Motor Retraining
- Exercises emphasising smooth, controlled movements
- Biofeedback-assisted training
- Task-specific training for problematic movements
Important note: Cervical dystonia exercises work best when combined with other treatments and tailored by a physical therapist familiar with dystonia.
Botulinum Toxin Therapy (Botox and Alternatives)
Botulinum toxin injection therapy is the gold standard for cervical dystonia treatment in the United States, with FDA approval since 1989 for this indication.
Understanding Botox: Mechanism and Function
Botox, the brand name for botulinum toxin type A, works by inhibiting the release of acetylcholine at the neuromuscular junction, which leads to temporary muscle relaxation. This targeted mechanism makes it highly effective for managing the involuntary contractions seen in cervical dystonia. In clinical use, Botox drugs treat chin dimpling, cervical dystonia, and bunny lips by reducing excessive muscle activity and improving overall muscle control, helping patients experience relief from stiffness, abnormal postures, and discomfort.
Botox Allergan 50 Unit Dosing
The standard Botox Allergan 50 unit formulation is frequently used, though actual doses vary:
- Typical dosing range: 25-50 units per muscle site
- Total injection: Often 100-200+ units across multiple muscles
- Frequency: Injections required every 12-16 weeks for sustained benefit
- Cost in the USA: Typically $300-600 per injection session (often not covered by insurance despite FDA approval)
Botox Half-Life and Duration of Action
Understanding Botox's half-life helps predict treatment duration:
- Botox half-life: Approximately 3-4 days (meaning the toxin degrades with this timeline)
- Clinical onset: Symptom improvement begins at 3-5 days
- Peak effect: Achieved at 2-3 weeks
- Duration: Benefits typically last 12-16 weeks
- Rebound timeline: Symptoms gradually return as the toxin degrades
The relatively short Botox half-life necessitates regular injections, making it a long-term commitment for most patients.
Toxin Brands Available in the USA
Multiple toxin brands offer botulinum toxin therapy options:
-
Botox (Allergan/AbbVie): Type A toxin, most established track record, botox class name is onabotulinumtoxinA
- FDA approved for cervical dystonia
- Dosing: Measured in units specific to Botox
-
Dysport (Ipsen): Type A toxin, different molecular formulation (abobotulinumtoxinA)
- More spreadable formulation
- Dosing: 2.5-3x higher unit count than Botox
- Faster onset (24-48 hours vs 3-5 days)
-
Xeomin (Merz): Type A toxin (incobotulinumtoxinA)
- No protein coating (different formulation)
- Similar onset and duration to Botox
- May have lower antibody formation risk
-
Jeuveau (Evolus): Newer type A formulation (prabotulinumtoxinA)
- Approved for cosmetic use, increasingly used off-label
- Similar characteristics to other type A toxins
Botox CNS Penetration and Controlled Substance Status
Botox CNS: One important clinical consideration is that botulinum toxin does NOT cross the blood-brain barrier to any clinically significant degree. This means the therapeutic effect is purely peripheral (local to the muscles), not central nervous system mediated. This explains why botox works for movement disorders while avoiding many CNS-related side effects.
Is Botox a controlled substance? No. While botulinum toxin is one of the most potent neurotoxins known, Botox's controlled substance status is negative—it is not scheduled as a controlled substance by the DEA. It is classified as a prescription medication requiring FDA approval and physician administration.
Oral Medications
- Anticholinergics: Trihexyphenidyl, benztropine (older medications, limited effectiveness for cervical dystonia)
- Muscle relaxants: Baclofen, cyclobenzaprine (modest benefit)
- Benzodiazepines: Clonazepam, diazepam (for anxiety and muscle tension)
- Beta-blockers: Propranolol (for tremor component)
Surgical Options
For severe cases unresponsive to botox and medications:
- Deep Brain Stimulation (DBS): Implanted devices that modulate abnormal brain circuits
- Selective denervation: Surgical severing of nerve pathways to dystonic muscles (less common now)
How I Cured My Cervical Dystonia: Real Patient Stories and Insights
While "cured" is rarely the right word—cervical dystonia is typically a chronic condition requiring ongoing management—many patients achieve remarkable symptom control and improved quality of life.
Common Treatment Success Patterns
Patient Case 1: Sarah's Botox Success Sarah, a 42-year-old from Boston, noticed early warning signs before severe cervical dystonia developed when her head began tilting slightly during stressful workdays. "At first, I thought it was just tension," she recalls. After diagnosis, she started Botox treatment with Allergan 50-unit injections every 12 weeks. "Within three weeks of my first injection, the improvement was dramatic. I went from being self-conscious about my posture to feeling confident again. I'm not cured, but I'm living my life."
Patient Case 2: Michael's Multimodal Approach Michael combined cervical dystonia exercises prescribed by a dystonia-specialised physical therapist with oral medications and eventually Botox. "The exercises helped me understand my body's patterns," he explains. "I learned sensory tricks that work for me—touching my chin or forehead provides temporary relief. Between the exercises, my medications, and botox injections, I've gone from severe disability to managing mild symptoms most days."
Key to Success: Most successful outcomes involve:
- Early diagnosis and treatment initiation
- Finding experienced dystonia specialists
- Combining multiple treatment modalities
- Consistent physical therapy and exercise
- Psychological support for adjustment
- Patient persistence in finding the right medication or injection protocol
Cervical Dystonia in America: USA-Specific Information
Prevalence in the United States
- An estimated 11,000-60,000 Americans have cervical dystonia (exact numbers uncertain)
- Affects men and women equally
- Peak onset: 40-50 years old, but can develop at any age
- Often takes 1-3 years from symptom onset to diagnosis (diagnostic delay is common)
Accessing Specialised Care in the USA
Finding the right specialist:
- Movement disorder neurologists (fellowship-trained specialists)
- Universities and major medical centres often have dystonia specialists
- Dystonia Medical Research Foundation maintains a physician referral directory
- Telemedicine options increasingly available
Insurance and Cost Considerations in America
- Botox for cervical dystonia is FDA-approved, but frequently not covered by insurance
- Medicare coverage varies by regional carrier
- Out-of-pocket costs typically $300-600 per injection session
- Physical therapy: Often covered with an appropriate referral
- Medications: Usually covered if medically necessary
Dystonia Advocacy and Support in the USA
- Dystonia Medical Research Foundation: National nonprofit organisation providing resources, research funding, and support groups
- Patient support groups: Both in-person and online communities for emotional support and information sharing
- Clinical trials: Opportunities to access new treatments through research studies
Living Well with Cervical Dystonia
Practical Daily Life Strategies
Managing at work:
- Communicate with your employer about your condition
- Arrange ergonomic assessments and desk modifications
- Schedule breaks for stretching and relaxation
- Consider flexible work arrangements
- Utilise employee assistance programs for counselling
Social and emotional health:
- Connect with support groups (online and in-person)
- Work with a therapist experienced with chronic illness adjustment
- Practice self-compassion—this is not your fault
- Educate friends and family about your condition
- Focus on activities that bring joy and normalcy
Optimising treatment:
- Keep detailed symptom diaries to track patterns
- Maintain consistent physical therapy routines
- Attend regular follow-up appointments with specialists
- Communicate openly with your treatment team about side effects or inadequate symptom control
- Stay informed about new treatment developments
The Importance of Specialised Care
Working with providers experienced in cervical dystonia significantly improves outcomes. Movement disorder neurologists understand the complexities of dystonia and can optimise treatment plans in ways general practitioners cannot. The investment in finding and working with a specialist pays dividends in quality of life improvements.
Research and Future Directions
The understanding of cervical dystonia etiology continues to advance. Current research explores:
- Genetic mutations underlying primary dystonia
- Neuroimaging to understand brain circuit abnormalities
- Development of new and improved botulinum toxin formulations
- Gene therapy approaches
- Novel medications targeting specific neurochemical pathways
- Advanced deep-brain stimulation techniques
Participating in research through clinical trials not only advances the field but also provides access to cutting-edge treatments.
FAQ
Q: Can cervical dystonia go away on its own?
A: Spontaneous remission is rare, occurring in less than 10% of cases. While some people experience symptom fluctuations, complete resolution without treatment is uncommon. Early intervention and consistent treatment provide the best chances for symptom control.
Q: How often do I need Botox injections?
A: Most patients require injections every 12-16 weeks. The Botox half-life means effects gradually diminish, necessitating regular treatment to maintain symptom control. Some patients develop antibodies to the toxin, requiring brand switching or higher doses.
Q: Are there any cures for cervical dystonia?
A: Currently, no cure exists. However, treatments effectively manage symptoms and restore quality of life for many patients. Research into gene therapy and new neurological understanding continues to advance treatment options.
Q: What cervical dystonia exercises should I do?
A: Cervical dystonia exercises should be specifically tailored to your pattern of movement and designed by a physical therapist experienced with dystonia. Avoid forceful stretching, which can increase dystonia. Focus on gentle, controlled movements and sensory motor retraining.
Q: Can stress make cervical dystonia worse?
A: Absolutely. Stress is one of the most common exacerbating factors. Many patients develop strategies like relaxation techniques, yoga, meditation, and stress management counselling to help control stress-related symptom flares.
- Art
- Causes
- Crafts
- Dance
- Drinks
- Film
- Fitness
- Food
- Spellen
- Gardening
- Health
- Home
- Literature
- Music
- Networking
- Other
- Party
- Religion
- Shopping
- Sports
- Theater
- Wellness


